PATHOLOGY
Asthma
- Asthma is a disease caused by reversible bronchoconstriction caused by airway hyper-responsiveness to a number of stimuli
- Atopic asthma is caused by a TH2 and IgE mediated immune reaction
- eosinophils are key inflammatory cells involved
- also mast cells, neutrophils and lymphocytes
- eosinophils are key inflammatory cells involved
- Airway remodelling is irreversible in chronic asthma leading to COPD
- fibrosis of the basement membrane
- smooth muscle hyperplasia
- gland hypertrophy
|
The one that is blocked by mucus (jelly-like) is the airway
The other two are artery/vein |
Restrictive Lung Diseases
In a typical alveolus, 99% of the lumen is covered by Type 1 pneumocytes which are responsible for gas exchange. Type II cells are responsible for producing surfactant that reduces the surface tension inside the alveolus to keep the lumen patent. The interstitium is the tissue between each alveolus and the adjacent capillary and contains myofibroblasts, collagen and elastin. With chronic stimulation and inflammation of this tissue, more collagen is deposited, leading to interstitial fibrosis.
Interstitial fibrosis affects the ability of the body to exchange carbon dioxide and oxygen in the lungs.
Restrictive lung diseases are characterised a reduction in total lung capacity and by a normal-increased FEV1/FVC ratio on spirometry. The reduction in lung capacity can be attributed to:
These conditions have non-specific symptoms which can make early diagnosis difficult, but lead to irreversible fibrosis, at which point symptoms become more apparent and the issue can be more easily diagnosed.
Oftentimes, exposure to these harmful particles is occupational. The risk of developing more severe lung conditions is also compounded by the amount of air pollution in the general region that an individual is exposed to in daily life.
Interstitial fibrosis affects the ability of the body to exchange carbon dioxide and oxygen in the lungs.
- Thickened alveolar wall → decreased gas exchange
- Oxygen exchange is particularly impaired as oxygen is much less soluble in plasma than carbon dioxide, which means that any change to wall thickness will particularly affect the oxygen.
- reduced lung compliance → decreased alveolar ventilation
- fibrosis → decreased gas diffusion
Restrictive lung diseases are characterised a reduction in total lung capacity and by a normal-increased FEV1/FVC ratio on spirometry. The reduction in lung capacity can be attributed to:
- Reduced movement of the chest wall (paralysis, obesity) = reduced lung compliance
- Interstitial lung diseases
- pneumoconiosis
- idiopathic pulmonary fibrosis (fibrosis of unknown cause)
- infections
- drug-induced
- infiltrative lung diseases (pneumonitis; inflammation of the alveolar wall)
These conditions have non-specific symptoms which can make early diagnosis difficult, but lead to irreversible fibrosis, at which point symptoms become more apparent and the issue can be more easily diagnosed.
Oftentimes, exposure to these harmful particles is occupational. The risk of developing more severe lung conditions is also compounded by the amount of air pollution in the general region that an individual is exposed to in daily life.
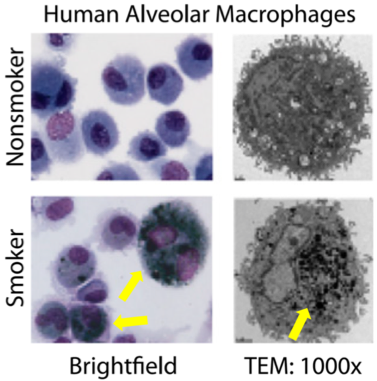
- When a dust particle or chemical enters the alveolus, it will be engulfed by resident macrophages. These macrophages will attempt to migrate to lymph nodes to clear the presumed "pathogen"
- on their journey, macrophages that have engulfed dust particles may get stuck in tissue, and die on the way, leading to inflammation that can eventually cause pneumoconiosis
- The size, shape and chemistry of the particle determines the place at which the macrophage will settle
- The amount of dust retained in the airways is proportional to the amount of tissue pathology that can be observed
- affected by clearance mechanisms, duration of exposure and the amount of dust in the air
- There are multiple complications of pneumoconiosis:
- loss of respiratory function
- fibrosis → loss of elasticity
- pleuritic adhesions
- emphysema
- pleural effusions
- Cardiovascular complications
- pulmonary hypertension
- cor pulmonale
- left-sided heart failure
- Infections (TB, bacterial) & pneumonia
- Malignancy (squamous cell carcinoma, mesothelioma)
- loss of respiratory function
|
Asbestosis
|
|
|
Silicosis
|
|
|
Coal Worker's Pneumoconiosis
|
|
- Initially, the coal dust is taken up by tissue macrophages in an attempt at a clearance mechanism
- Neutrophils and lymphocytes infiltrate and stimulate collagen production by fibroblasts which then leads to fibrosis of the interstitial tissue which will be heavy in these collagen deposits
- Surrounding alveoli will also be destroyed by the fibrosis and immune response
- Neutrophils and lymphocytes infiltrate and stimulate collagen production by fibroblasts which then leads to fibrosis of the interstitial tissue which will be heavy in these collagen deposits
Mesothelioma
- Mesothelioma is a cancer of the mesothelium; it is not classified as a lung cancer as it does not originate in the lung parenchyma
|
Lung Anthracosis
|
|
Pathology Related to Smoking
|
- Lung cancer is the #1 cancer killer
- Makes up 15% of cancer diagnoses but 25-30% of cancer deaths
|
Atherosclerosis
|
|
Thromboangiitis Obliterans (Buerger's Disease)
|
|
|
|
- Some of the adducts can be repaired, others will lead to mutations in oncogenes and tumour suppressor genes
- A single cancer can contain over 2000 mutations
- Most of these will not cause cancer
- A handful of driver genes will be responsible for the malignancy
- This will then cause deregulation of cell growth control → cancers
- A single cancer can contain over 2000 mutations
- Nicotine also contributes to cell growth pathways and can cause a loss of control over cellular proliferation
- Some carcinogens cause organ-specific pathology:
- Polycyclic aromatic hydrocarbons → lung/laryngeal/oral cavity cancers
- NNK → lung/laryngeal/pancreatic/oral cavity cancers
- Polonium 210 in snuff → lung/larynx/oral cavity cancers
- NNN in snuff and tobacco→ oesophageal/oral cavity cancers
- 2-naphthylamine → bladder cancer
- Smoking also potentiates the risk of other carcinogen exposure beyond their individual risks:
- Alcohol → 5x risk of laryngeal cancer
- Smoking → 8x risk of laryngeal cancer
- Alcohol + Smoking → 45x risk of laryngeal cancer
- Asbestos → 5x risk of lung cancer
- Smoking → 10x risk of lung cancer
- Smoking + asbestos → 55x risk of lung cancer
- Cigarette exposure has profound effects on all age groups:
- Foetal: hypoxia in mothers smoking around 10/day, low birth weight, prematurity, spontaneous abortion, premature membrane ruptures, placenta praevia, abruptio placentae
- Children: middle ear disease, respiratory symptoms, LRTI, SIDS (sudden infant death syndrome)
- Adults: nasal irritation, lung cancer, coronary artery disease, low birth weight babies in women who smoke
|
Emphysema
|
|
|
Interstitial Lung Disease
|
Pneumonia
|
Lobar Pneumonia
1) Congestion - 24 hours
|
Red Hepatisation
Grey Hepatisation
Lobar pneumonia of middle right lobe
Upper right lobar pneumonia
|
|
Bronchopneumonia
|
|
Lung Cancer
- Lung cancer is the 4th most common cancer in Australian men and women
- Incidence increases with age (huge increase after age 40, exponential after age 60)
- The number of females diagnosed with lung cancer has doubled in the last 20 years
- Incidence in males is higher overall
- The 5-year survival rate for lung cancer decreases with age and is far worse than for other malignancies
- Absolute survival = percentage of people diagnosed who are still alive after 5 years
- Relative survival = percentage of people diagnosed who are still alive after 5 years accounting for age and gender
- 10% in males, 15% in females for lung cancer
- Mortality: Incidence ratio = how many people die out of how many new cases are diagnosed
- Australia has one of the lowest ratios in the world with all cancers
|
Squamous Cell Metaplasia
|
- Can result in decreased ability to function or increased propensity for malignant transformation
- E.g. loss of ciliation due to cilia toxins in smoke → increased infection rates as decreased mucous clearance
|
Squamous Cell Carcinoma (E4-1)
|
|
Adenocarcinoma
|
|
|
Small Cell Carcinoma
|
|